COVID-19: Implications and Guidance for Patients Treated with Immunotherapy
2020-03-20
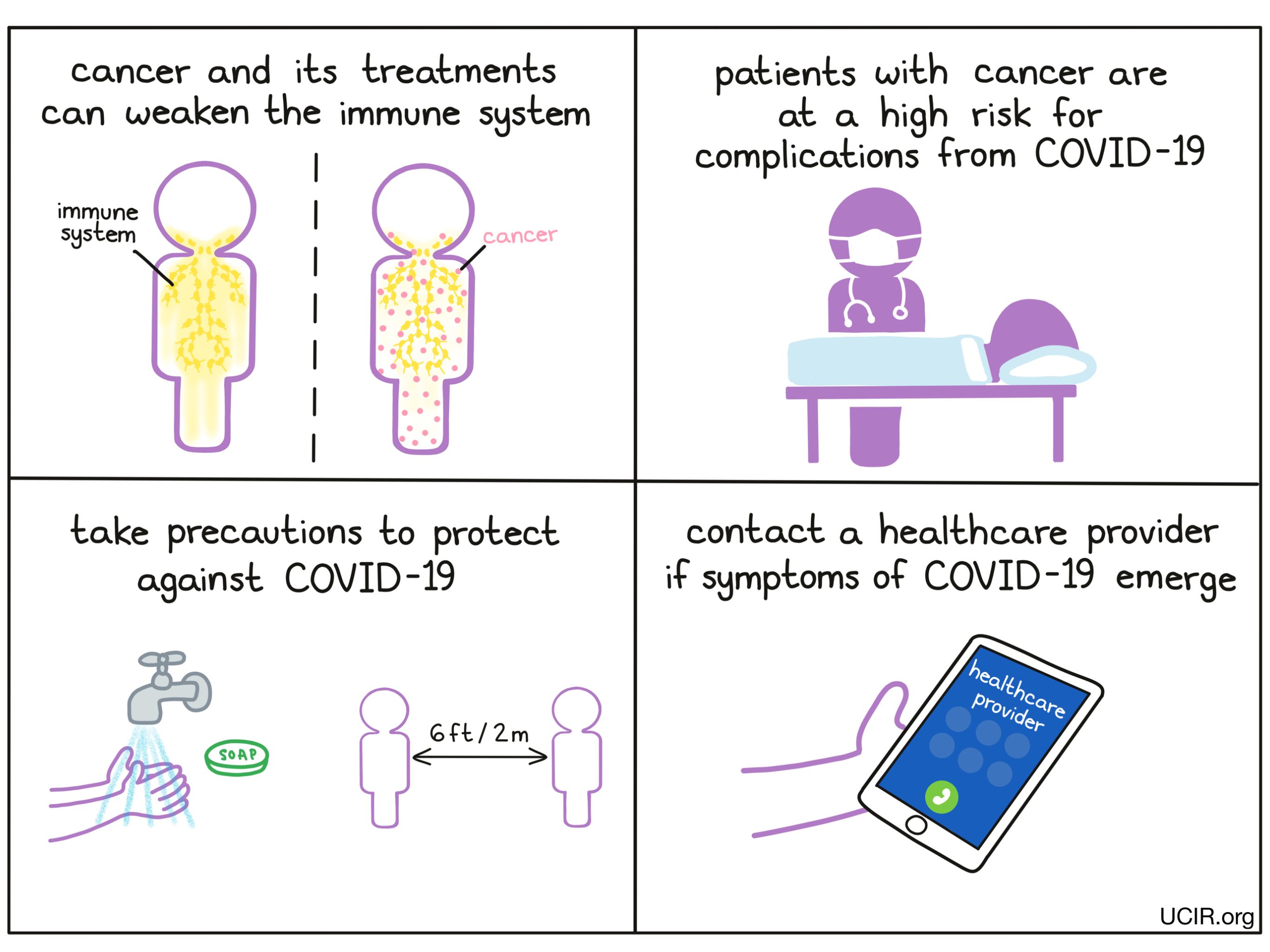
The novel coronavirus COVID-19 is considered a pandemic by the World Health Organization. While the majority of people infected with COVID-19 experience mild to moderate symptoms, including cough, fever, and shortness of breath, others experience severe, life-threatening complications. Those most at risk of such complications include the elderly and people with certain health conditions that hinder their ability to fight off infections – including patients with cancer and some survivors of cancer. Patients in high-risk categories should take extra precautions to protect themselves from COVID-19 and should contact their healthcare provider immediately if symptoms of COVID-19 emerge.
How does cancer and the treatment of cancer affect a patient’s risk of infection?
Cancer and its treatments put patients at an increased risk of infection. Cancer puts stress on the body and on the immune system, which lowers the immune system’s ability to fight off invaders like viruses and bacteria. Patients with blood cancer are particularly vulnerable to infections, as their disease specifically affects immune cells. Certain treatments, like chemotherapy, steroids, and bone marrow transplants, affect the immune system directly, leaving patients partially or fully immunocompromised and at a very high risk of infection. Treatments like radiation and surgery may also indirectly lower the immune system’s capabilities. Patients with cancer who are over 65 years old or who have additional high-risk illnesses are at a further increased risk.
How does cancer immunotherapy affect the risk of infection?
Immunotherapy works by altering a patient’s immune system to enhance immune responses against cancer. Different immunotherapies affect the immune system in unique ways, and while the immune response to cancer may be increased, it is not always clear what effects immunotherapy may have on immune responses to threats like infections. Therefore, patients undergoing immunotherapy or who have undergone immunotherapy should follow the same precautions as others who are considered at a higher risk for serious illness from COVID-19.
What is being done to stop the spread of COVID-19 to patients with cancer?
Around the globe, governments, medical facilities, communities, and individuals are taking precautions to prevent the spread of COVID-19. Many hospitals and doctor’s offices are implementing preventative strategies including screening patients (by telephone and in person) for signs of COVID-19, restricting non-essential visitors, and rescheduling or postponing non-essential appointments or making telehealth appointments available. This may include some long-term follow-up appointments if they are not considered medically urgent. Even appointments for patients enrolled in clinical trials are being conducted only if critical to the needs of the patients and the trial. Patients with plans to travel to receive care or to participate in clinical trials should contact their providers for guidance.
How can patients with cancer protect themselves from COVID-19?
Patients with cancer and their caregivers should follow government guidelines for high-risk groups. The United States Centers for Disease Control (CDC) recommends:
- frequent and thorough handwashing,
- frequent household cleaning and disinfecting,
- avoiding high-touch surfaces (elevator buttons, door handles, handrails) in public places,
- avoiding touching your face with unwashed hands,
- avoiding crowds,
- avoiding non-essential travel,
- physically distancing yourself from others (whether they appear sick or not), and
- staying home as much as possible.
Patients who are currently at home should stock up on supplies, including prescription and over-the-counter medications, medical supplies, household necessities, and groceries in order to remain at home for as long as may be necessary. Further, patients who rely on caregivers should have a plan in place in the event that their caregiver gets sick. If a patient with cancer is in the hospital, they should follow hospital guidelines. Visitors should be limited regardless of whether they are showing symptoms of COVID-19.
In regards to any upcoming appointments, it is advisable to call the health care provider ahead of time. Some providers may recommend telehealth appointments in place of in-person appointments, may reschedule non-essential visits, or may provide further guidance on how to minimize risk if an in-person visit is necessary.
What should patients with cancer and caregivers do if they have or suspect they have COVID-19?
Anyone who thinks they may have COVID-19 should call their healthcare provider immediately. COVID-19 symptoms include fever, cough, and shortness of breath. Patients in high-risk groups with suspected or confirmed cases of COVID-19 should remain in contact with their healthcare providers to monitor symptom progression. Most of the time, symptoms can be managed at home, but severe symptoms may need to be managed in a hospital setting. Emergency warning signs of COVID-19 include difficulty breathing or shortness of breath, persistent pain or pressure in the chest, new confusion, inability to arouse, or bluish lips or face. Appearance of any of these symptoms demands immediate medical attention. If an urgent care or emergency room visit is necessary, it is advisable to call ahead so that staff can prepare. The CDC also recommends that current and former patients with cancer stay in touch with friends, family, and neighbors, and develop an emergency plan in case they become sick and need to ask for help.
by Lauren Hitchings
References:
https://www.cdc.gov/coronavirus/2019-ncov/specific-groups/high-risk-complications.html
https://www.cancer.org/latest-news/common-questions-about-the-new-coronavirus-outbreak.html
https://www.cancer.gov/contact/emergency-preparedness/coronavirus
https://www.thelancet.com/journals/lanonc/article/PIIS1470-2045(20)30149-2/fulltext




