How is the drug name pronounced?
Breyanzi: bray-an-zee
Lisocabtagene Maraleucel: LIH-soh-KAB-tuh-jeen MAR-uh-LOO-sel
What cancer(s) does this drug treat?
Breyanzi is approved for:
Large B-cell lymphoma
Chronic lymphocytic lymphoma (CLL)
Follicular lymphoma (FL)
Mantle cell lymphoma (MCL)
Large B-cell lymphoma
Breyanzi is approved for:
-
Patients with large B-cell lymphoma, including diffuse large B-cell lymphoma (DLBCL), high-grade B-cell lymphoma (HGBCL), primary mediastinal large B-cell lymphoma (PMBCL), and follicular lymphoma (FL) grade 3B,who:
- were previously treated with chemoimmunotherapy, but the disease did not respond or came back within 12 months of therapy, OR
- were previously treated with chemoimmunotherapy, but the disease stopped responding or came back after 12 months of therapy, and the patient cannot be treated with hematopoietic stem cell transplantation, OR
- were previously treated with at least two different types of therapy by mouth or injection into the vein (i.v.), but the cancer either did not respond to treatment, or has since returned.
Chronic lymphocytic leukemia (CLL)
Breyanzi is approved for:
- Patients with chronic lymphocytic leukemia (CLL) or small lymphocytic lymphoma (SLL) who have previously been treated with at least 2 prior lines of therapy, including a BTK inhibitor and a BCL-2 inhibitor, but either did not respond or their disease has come back.
Follicular lymphoma (FL)
Breyanzi is approved for:
- Patients with follicular lymphoma (FL) who have previously been treated with at least 2 prior lines of systemic therapy, but either did not respond or their disease has come back.
Mantle cell lymphoma (MCL)
Breyanzi is approved for:
- Patients with mantle cell lymphoma (MCL) who have previously been treated with at least 2 prior lines of therapy, including a BTK inhibitor, but either did not respond or their disease came back.
Limitations of Use
Age: The safety and efficacy of Breyanzi in patients under 18 years of age have not been established.
Pregnancy/Breastfeeding: The risks associated with Breyanzi during pregnancy are not known and cannot be ruled out. Due to the potential for harm to the fetus, Breyanzi is not recommended for use during pregnancy. The risks associated with Breyanzi during breastfeeding are not known and cannot be ruled out. Due to the potential for adverse reactions in the breastfed child, women are advised not to breastfeed during treatment with Breyanzi.
Primary central nervous system lymphoma: Breyanzi should not be used for the treatment of patients with primary central nervous system lymphoma.
Effects on the ability to drive : Patients are advised to refrain from driving for at least 2 weeks after receiving Breyanzi.
Vaccinations: Live virus vaccinations (e.g., chickenpox or measles, mumps, and rubella (MMR)) are not recommended for at least 6 weeks prior to or during Breyanzi treatment, and until the patient’s white blood cell count has recovered following treatment.
Corticosteroids: Corticosteroids should not be administered shortly before Breyanzi treatment, as they may limit the activity of Breyanzi.
What type of immunotherapy is this?
- CAR T Cell Therapy
How does this drug work?
Target:
- CD19 on B cells
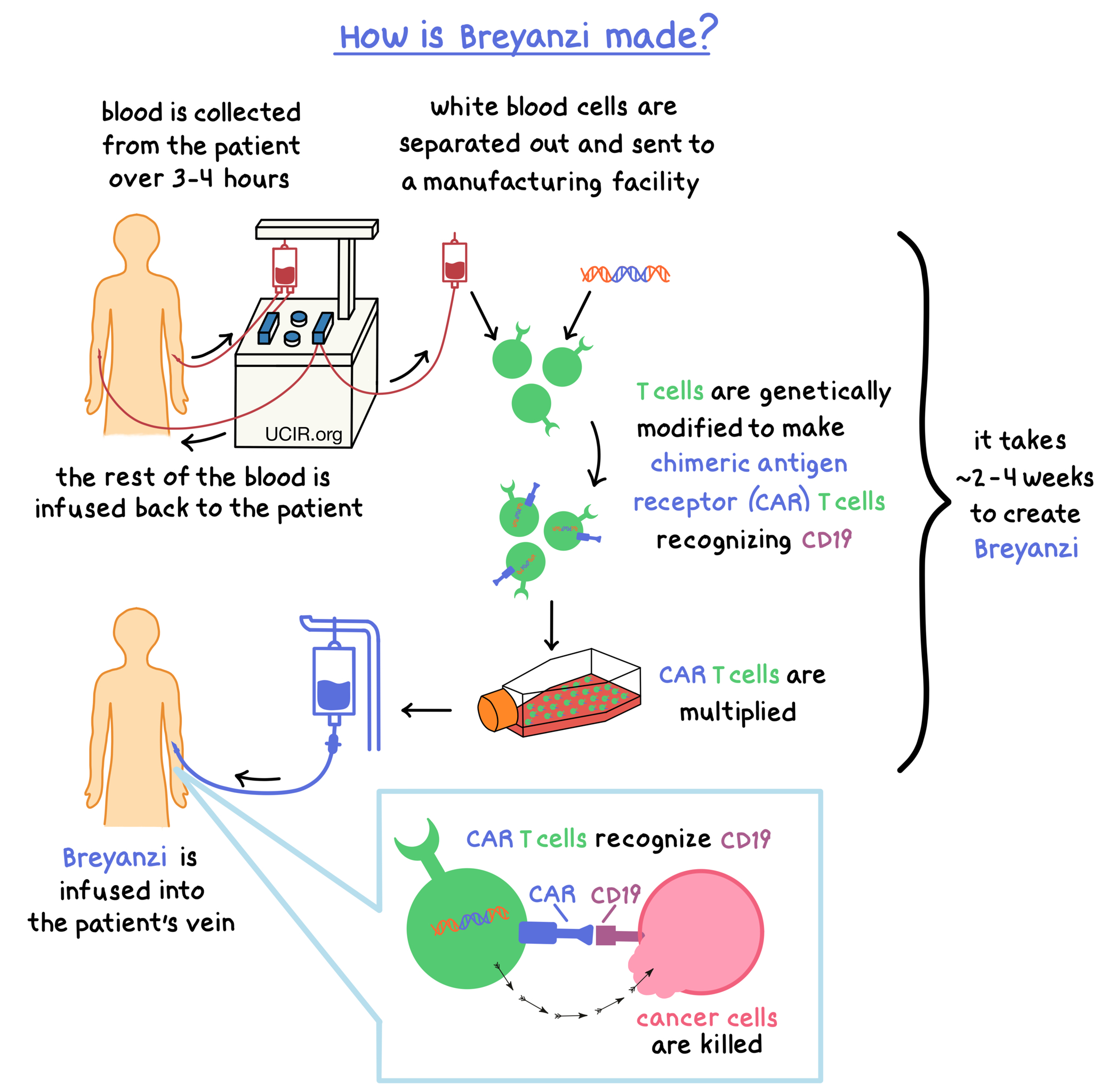
Breyanzi is made from the patient’s own T cells (a type of white blood cell). In order to make Breyanzi, blood is collected from the patient’s vein – this process usually takes 3 to 4 hours. In a process called leukapheresis, the white blood cells (including T cells) are separated from the collected blood, and the rest of the blood is returned to the patient. The collected white blood cells are sent to a specialized manufacturing facility where the patient’s T cells are genetically modified in such a way that they make a protein on their surface called a chimeric antigen receptor (CAR). The modified T cells (“CAR T cells”) are multiplied to create millions of CAR T cells.
The CAR on the surface of the modified T cell can attach to a protein called CD19 on the surface of the cancer cell. When a CAR attaches to CD19, T cells recognize the cancer cells and kill them. The entire process to create Breyanzi from the collected blood could take approximately 2 to 4 weeks.
How is this drug given to the patient?
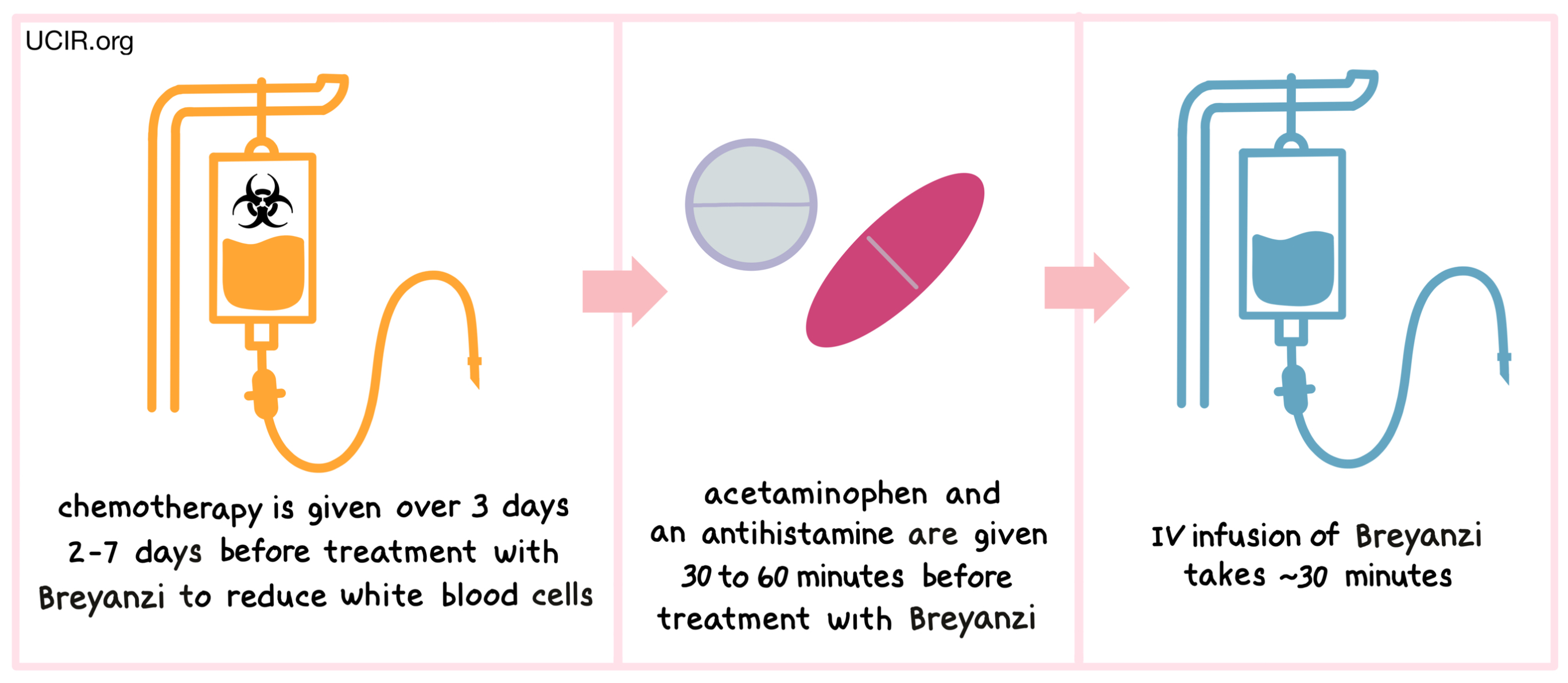
Before receiving Breyanzi, patients are treated with a short course of cyclophosphamide and fludarabine chemotherapy to reduce the number of white blood cells in their system. Cyclophosphamide and fludarabine are administered over 3 days through a tube in the vein (intravenous, i.v.), 2 to 7 days prior to treatment with Breyanzi. The reduction in the patient’s white blood cell count gives the CAR T cells in Breyanzi enough space to multiply, and provides them with the resources needed to survive longer in the patient. About 30 to 60 minutes before receiving Breyanzi, patients receive acetaminophen and an antihistamine (e.g., diphenhydramine) to reduce the chance of reactions to the infusion.
Patients receive Breyanzi through an intravenous (i.v.) infusion. The administration of Breyanzi usually takes about 30 minutes.
Patients are monitored daily for at least 7 days following administration of Breyanzi, and should plan to stay close to the treatment location for at least 2 weeks after receiving Breyanzi.
What are the observed clinical results?
For: Large B-cell lymphoma
Chronic lymphocytic lymphoma (CLL)
Follicular lymphoma (FL)
Mantle cell lymphoma (MCL)
It is important to keep in mind that each patient’s actual outcome is individual and may be different from the results found in the clinical studies.
Large B-Cell lymphoma
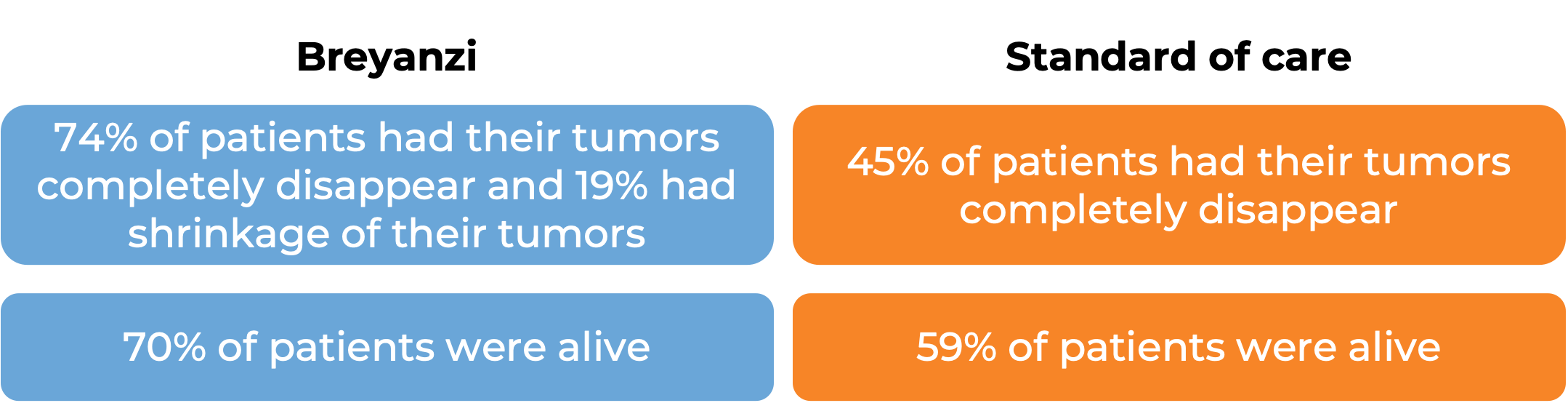
In a clinical trial, 184 patients with large B-cell lymphoma who had previously been treated with first-line chemoimmunotherapy, but their cancer either did not respond or came back within 12 months, were treated with Breyanzi or standard therapy. At a median follow-up of 6 months:
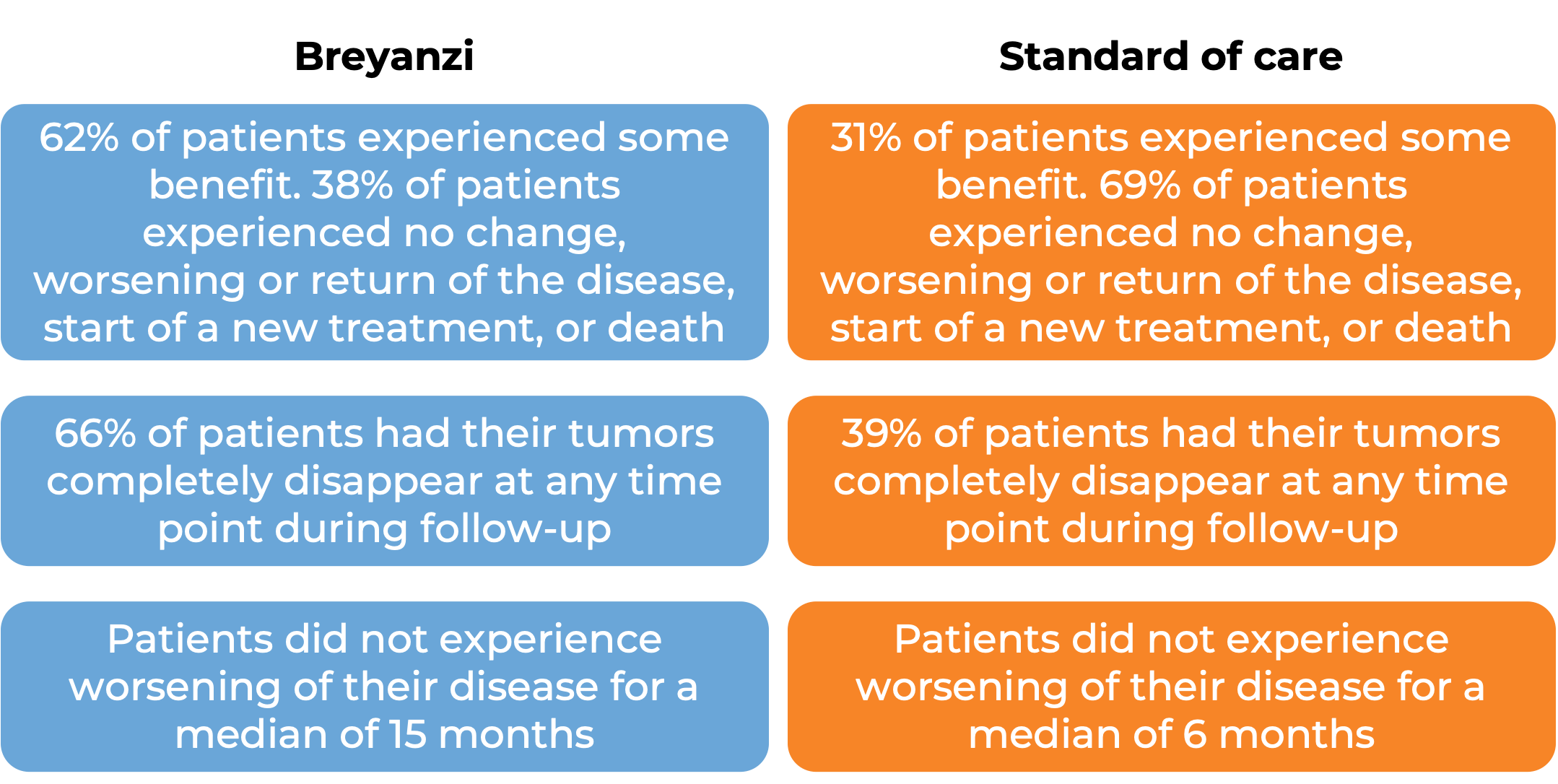
In another clinical trial, 61 patients who were previously treated with first-line chemoimmunotherapy, but the disease stopped responding or came back, and who could not receive hematopoietic stem cell transplantation, were treated with Breyanzi. At a median follow-up of 12 months:

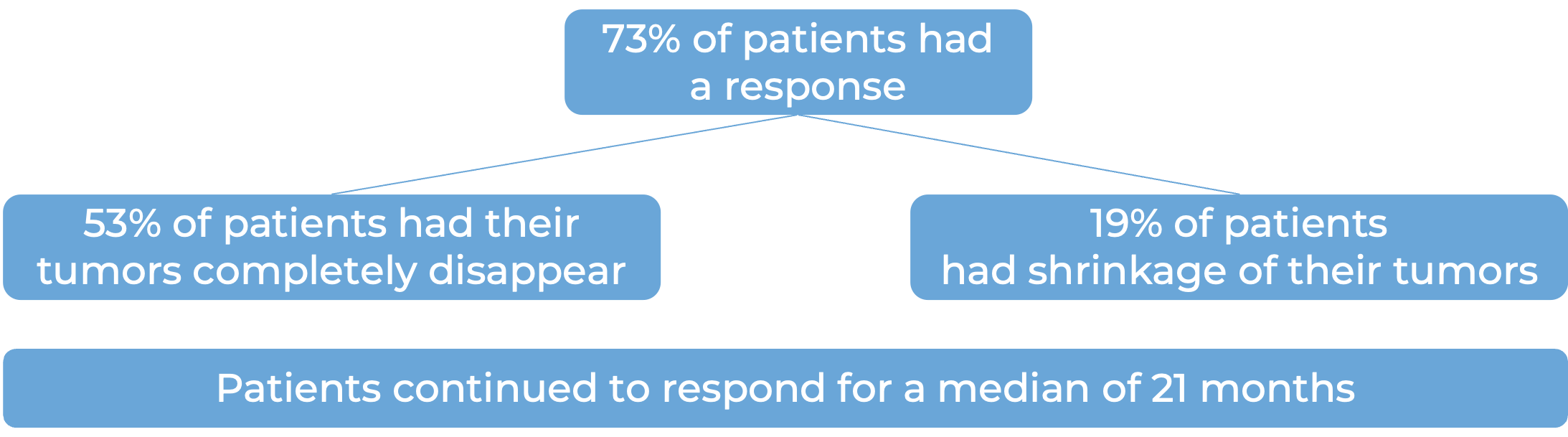
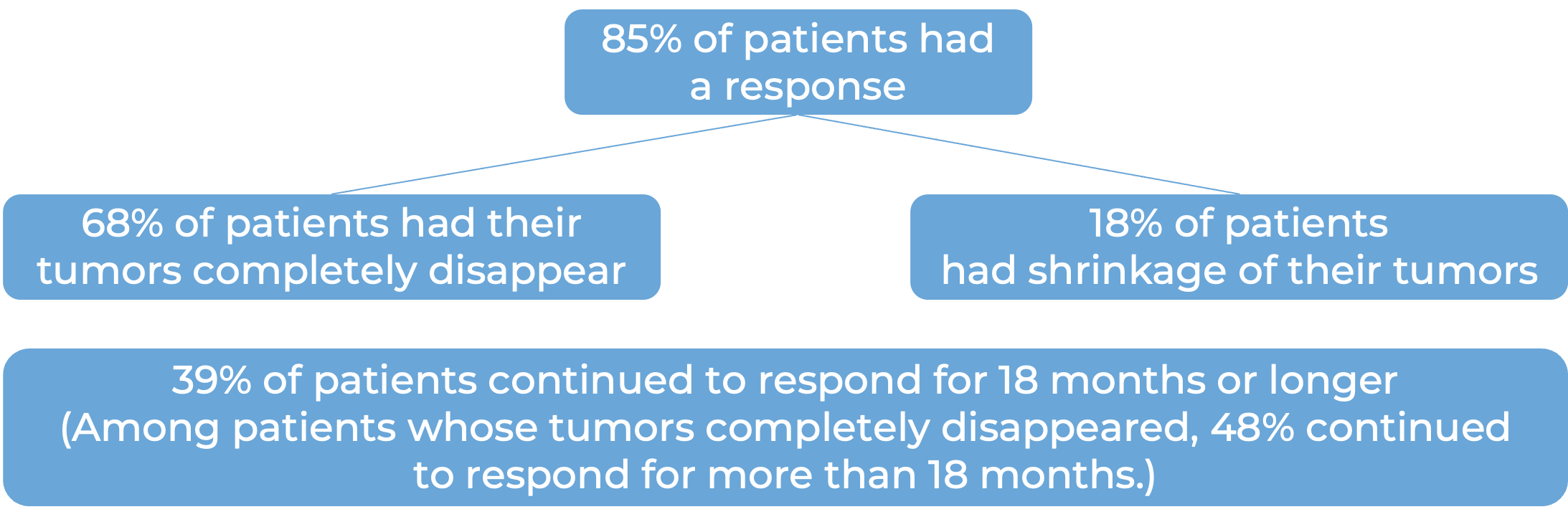
In another clinical trial, 192 patients with large B-cell lymphoma whose cancer either did not respond (refractory) or had returned (relapsed), were treated with Breyanzi.

Chronic lymphocytic lymphoma (CLL) or small lymphocytic lymphoma (SLL)
In a clinical trial, 65 patients with chronic lymphocytic leukemia (CLL) or small lymphocytic lymphoma (SLL) who were previously treated with at least 2 prior lines of therapy, including a BTK inhibitor and a BCL-2 inhibitor, but either did not respond or their disease came back, were treated with a full dose of Breyanzi.
Follicular lymphoma (FL)
In a clinical trial, 94 patients with follicular lymphoma (FL) who were previously treated with at least 2 prior lines of systemic therapy, but either did not respond or their disease came back were treated with a full dose of Breyanzi. At a median follow-up of 17 months:

Note: Rounding percentages after the decimal can cause inconsistencies between the total and the sum of the parts.
Mantle cell lymphoma (MCL)
In a clinical trial, 68 patients with mantle cell lymphoma (MCL) who were previously treated with at least 2 prior lines of therapy, including a BTK inhibitor, but either did not respond or their disease came back, were treated with a full dose of Breyanzi. At a median follow-up of 22 months:
Note: Rounding percentages after the decimal can cause inconsistencies between the total and the sum of the parts.
What are the potential side effects?
The most common side effects of Breyanzi include fever, cytokine release syndrome, fatigue, muscle and joint pain, nausea, coughing, vomiting, constipation, diarrhea, abdominal pain, headache, decreased appetite, dizziness, swelling, low blood cell counts, low blood pressure, and elevated heart rate. Some side effects, such as cytokine release syndrome (CRS), neurological toxicities, infections, and newly arising T cell blood cancers may be severe or life-threatening. Patients and caregivers receive careful instructions to monitor for signs and symptoms related to these side effects and the conditions are managed by the health care provider.
Cytokine release syndrome (CRS)
CRS is caused by a widespread release of molecules called cytokines, which are involved in inflammation and can affect the function of various organs. Cytokines may be released by the CAR T cells in Breyanzi or by other immune cells in the patient’s body. Signs and symptoms of CRS include high fever, chills, difficulty breathing, fast or irregular heartbeat, severe nausea, vomiting, diarrhea, very low blood pressure, low oxygen level, and dizziness or lightheadedness. CRS typically occurs between 1 and 15 days after Breyanzi infusion, and the health care provider should be immediately notified if symptoms occur.
Neurological toxicities
Some of the cytokines released during CRS can result in disruption of the blood-brain barrier, leading to the development of neurological toxicities. Symptoms of neurological toxicities include confusion, altered or decreased consciousness, tremors, seizures, headache, loss of balance, and difficulty speaking and understanding. Neurological toxicities typically occur about 8 days after Breyanzi infusion, but could occur up to 8 weeks after infusion.
Serious infections
Breyanzi can lead to other side effects, some of which could be long lasting. The CAR T cells in Breyanzi kill cancer cells that have the molecule CD19 on their surface; however, CD19 is also found on the surface of healthy B cells, which are also killed by Breyanzi. The decrease in healthy B cells leads to low levels of antibodies (immunoglobulins) and an increased risk of serious, potentially life-threatening, infections. If a patient is a carrier of the hepatitis B virus, Breyanzi can cause serious liver problems, including liver failure and death.
Interference with lab tests for HIV infection
Some lab tests for HIV infection may yield false-positive results in patients who have received Breyanzi.
Patients should report any symptoms to their healthcare provider, who can then initiate actions to limit or reverse the side effects. For a more complete list of possible side effects, see the full prescribing information.
Additional Information
Manufacturer
Bristol Myers Squibb
Approval
FDA and EMA
Links to drug websites
Other references
- Lisocabtagene maraleucel versus standard of care with salvage chemotherapy followed by autologous stem cell transplantation as second-line treatment in patients with relapsed or refractory large B-cell lymphoma (TRANSFORM): results from an interim analysis of an open-label, randomised, phase 3 trial. Kamdar M, et al. The Lancet (2022)
- Lisocabtagene maraleucel as second-line therapy in adults with relapsed or refractory large B-cell lymphoma who were not intended for haematopoietic stem cell transplantation (PILOT): an open-label, phase 2 study. Sehgal A, et al. The Lancet Oncology (2022)
Last updated on August 11, 2025